Setting reserves is a core responsibility of health actuaries. The mechanics are well documented, and actuaries generally apply sound methods—gathering credible data, reviewing payment patterns, monitoring operations, making working day adjustments—to ensure accurate estimates. Yet mature reserving practices can become a problematic area of actuarial practice. A perceived failure in the reserving process can damage the reputation of the actuarial department and jeopardize the career of senior actuaries.
Why does something so well understood create so much turmoil? The answer frequently resides not in the technical aspects of reserving, but in how results are communicated, understood and trusted.
When Good Methods Meet Unrealistic Expectations
Actuaries typically establish a reserving process that is disciplined and unbiased. Analysts routinely review claim payment timeliness, hospital billing practices and operational factors that influence development. Estimates are consistently tested, restated and documented.
The real problems often arise outside the spreadsheet. Executives and boards may expect a higher level of accuracy on restatements than is possible, or smooth financial results, even when emerging data show volatility. This can be at odds with reality since reserves are estimates, not certainties, and restatements are inevitable. Unrealistic expectations, coupled with opaque communication, can turn healthy variability into perceived failure. When reserving is allowed to become a “black box,” this can lead to misunderstandings.
From Black Box to Shared Understanding and Buy-in
Building a recurring, transparent communication process for reserves—one that shows how the estimate was set, where it sits within a reasonable range and how it has historically compared to actual outcomes—can be an effective practice. A structured Monthly Executive Reserve Note accompanied by a cross-functional management meeting can serve this purpose. Such a note and communication meeting convert technical detail into decision-ready management insight that auditors, board members and managers appreciate.
Recommended Executive Reserve Note Structure
Purpose
A monthly note can communicate the company’s reserve position and demonstrate adherence to disciplined actuarial practice. It can replace anxiety with clarity by providing the following:
- Transparency—Separate true operational performance (signal) from reserving and timing adjustments (noise).
- Discipline—Validate prior estimates and aim for a pattern of small, consistent favorable restatements, which reflects prudent, disciplined management. Conversely, a large negative restatement can raise financial alarms, making it harder to meet current-year targets and sparking pressure on finance teams.
- Clarity—Articulate where the current reserve sits within the range of reasonable results and how past estimates have developed against actual results.
Part 1: The Narrative (Main Report)
| Section | Content Focus | Management Value |
|---|---|---|
| I. Executive Summary & Reserve Position | State the booked reserve, its components (base incurred but not reported [IBNR] + explicit provision), and its placement in the actuarial range. | Can provide a quick confidence check—are reserves sound, and how much margin is held? |
| II. Core Performance: Medical Loss Ratio (MLR) & Trends | Present loss ratios and trends by major line of business, excluding current reserve changes. | Helps to separate underlying performance from accounting noise. |
| III. Reserve Movement & Reconciliation | Reconcile current to prior month reserves, show development on prior periods and summarize explicit provisions for known risk factors. | Helps to create a transparent audit trail while demonstrating disciplined reasoning. |
Part 2: Appendices (Technical Exhibits and Audit Support)
| Category | Attachment | Purpose |
|---|---|---|
| A. Core Validation | Lag-factor and payment pattern analyses; reserve restatement summaries; roll-forward reconciliations | To validate assumptions and provide an audit trail |
| B. Financial Accountability | Actual vs. budget revenue per member per month (PMPM), medical and pharmacy claims trends and premium deficiency testing | To link reserve levels to an early indicator of future company performance |
| C. Claims & Operations | Claims inventory metrics, analysis of special causes like provider billing interruptions or claims systems interruptions | To connect operational performance to reserve assumptions |
| D. Program Accruals | Detail on increasingly important risk-adjustment estimates, reinsurance and membership mix exhibits | To provide transparency for material financial accruals that impact company results |
Why It Matters
A consistent monthly note and communication meeting can help build confidence with both management and auditors, potentially reducing excessive scrutiny. Over time, this shifts reserve analysis from being a source of tension and uncertainty to an opportunity for improved transparency, discipline and control.
Emerging Issue
An increasingly significant challenge for reserving actuaries is the expectation that they will not only estimate incurred claim liabilities but also predict risk-adjustment revenue—a component that can be as large, volatile and operationally sensitive as the claim liability itself. Estimating risk adjustment revenue can be a more volatile process since it depends on an evolving ecosystem: company risk profiles potentially shifting year to year, government rules shifting, provider documentation practices varying, health plan product strategies and marketing efforts changing, and competitor behavior directly affecting final settlements as results are relative. These moving parts can complicate the process and can result in significant restatements.
Establishing a disciplined process—both for calculation and for communication—can help speak to observed variances. Some potential steps to explain the difficulty of estimating risk-adjustment factors include monitoring the volume and timing of codes submitted each month compared with prior years, reviewing coding patterns by provider group to identify operational delays and opportunities, and transparently conveying how emerging information shapes updated estimates. Though risk adjustment deserves a full paper of its own, the core message of this article remains consistent with the broader reserving framework: methods can be strengthened through the use of structured governance, repeatable communication and an early warning orientation to help leadership understand why estimates move and what actions may stabilize results.
Unique Challenges
Even with strong communication processes, actuaries sometimes face a deeper challenge, such as a senior financial leader who may not fully grasp the normal variability inherent in reserving. If restatements that fall within the bonds of normal variability are regularly interpreted as errors rather than as features of the process, the reserving function can become an undue burden on an actuarial staff.
If this occurs, the actuary could consider increasing communication instead of retreating. Actuaries can use the tools outlined in this article to present trends, ranges, operational drivers and historical performance—by line of business—in a consistent and repeatable format. As part of that dialogue, seeking to establish a shared understanding with senior leadership regarding the acceptable range of reserve restatements can help. Doing so can help to garner the support of senior leaders when estimates fall within the bounds of reasonable outcomes.
A second step is to seek peer review and share those findings with leadership. Engaging an experienced actuary—whether the company’s auditor or an external industry expert from a respected accounting or actuarial firm—to independently evaluate the company’s methods and assumptions can add value. A credible third-party validation of a sound process can help senior financial leaders and boards recognize that variability is normal and not evidence of actuarial error. While this peer review typically occurs as part of a year-end audit, it can be helpful to seek a second opinion if concerns emerge earlier in the year. Seeking timely peer review when these types of challenges arise can help validate the reserving approach and strengthen the credibility of the actuary’s work.
A third step is to seek to broaden understanding across the organization. Involving other executive leaders and the board can help spread awareness of the reserving process and potentially reduce the risk of an uninformed leader questioning otherwise disciplined work. When more people understand the inputs, outputs and operational constraints, this can help make the reserving process more transparent and more resilient.
And finally, actuaries would benefit from recognizing potential limits on the effectiveness of their communications. For example, if a senior financial leader has limited familiarity with insurance knowledge or reserving variability, it may be difficult for a communication strategy to take hold. In this type of situation, some professionals may consider whether this environment supports effective practice.
Final Thoughts
While not glamorous, health insurance reserving is a foundational element of a health insurer’s financial control system. Actuaries can help safeguard the balance sheet and their own credibility by coupling sound reserving methods with clear, regular communication. Avoiding unproductive focus on reserves allows leaders to concentrate on strategic business operations. Actuaries can make the reserving process appear simple, by investing in efforts that help key stakeholders understand how the uncertainty inherent in the reserving process is managed.
Practical Tips
- It can be helpful to get senior leadership input on acceptable ranges of restatements as a percentage of claims by major lines of business.
- Translating the prior period development amount as a percentage of the last 12 months of medical costs can also help. When viewed on this basis, it becomes clear that the month-over-month changes are relatively small.
- Many companies have outside auditors provide a quarterly view of their booked reserves relative to their independent range. This can provide a validation point if their company’s reserving process and results consistent with that of another independent practicing actuary’s. This external view can help leadership determine if their own company’s reserves were set at reasonable levels.
- It may be good to split out large claim reserve changes versus non-large claim reserve changes, mainly for commercial lines of business. Experienced leaders recognize that large-claim reserves naturally exhibit greater volatility than non-large claim reserves.
- To strengthen reserve accuracy, actuarial reserving teams can deepen communication with the claims, care management and revenue management teams. Actuaries benefit from linking as many operational metrics — claims trends, information technology, utilization, payment patterns, preauthorization data, computer system availability and pharmacy data—as possible to reserve outcomes, flagging any disconnects. By tailoring discussions to each stakeholder’s role, actuaries can help contribute to broader organizational understanding and allow each of the teams referenced earlier to contribute to more stable and data-driven results.
- For the future, as artificial intelligence becomes commonplace in many aspects of company processes, it may be wise to work with a data analytics team to determine if there are other data/methods that can help improve reserve accuracy.
- Work-day adjustments for the most recent months routinely explain much of the variation in claims runout experience. Simple things like the number of weekend days or the number of holidays can change actual monthly claims PMPM estimates by a few percentage points. Interestingly work-day adjustments can vary some by line of business and may differ significantly between dental and medical coverages.
- It can be helpful to graph lag factors. Health insurance actuaries traditionally use mathematical measures to establish lag factor estimates without graphing lag factors. However, in casualty insurance graphing lag factors can provide a critical check on reserve estimates.
The core value of this graphic approach is transparency. It can illustrate how claims payment factors vary by month and year, offering a visual record of changes in the underlying claims payment process over time. This can help executive leadership and auditors understand the reasonableness of reserve factors by seeing, for example, a documented slowdown in claims processing (like the 2024 Change Healthcare event), which can be used to justify specific reserve adjustments.
Furthermore, as completion factors increase, variability decreases. Graphs allow non-actuarial reviewers to have an educated opinion on the reserving staff’s picks and compare them to historical distributions, as shown in Figure 1. In addition, graphing lag factors can provide an early warning indicator if the claims process is speeding up or slowing down. Ultimately, graphing lag factors can help build confidence in the reserving process.
Figure 1
Hypothetical Factors Illustrating the Lag Factor Graphing Concept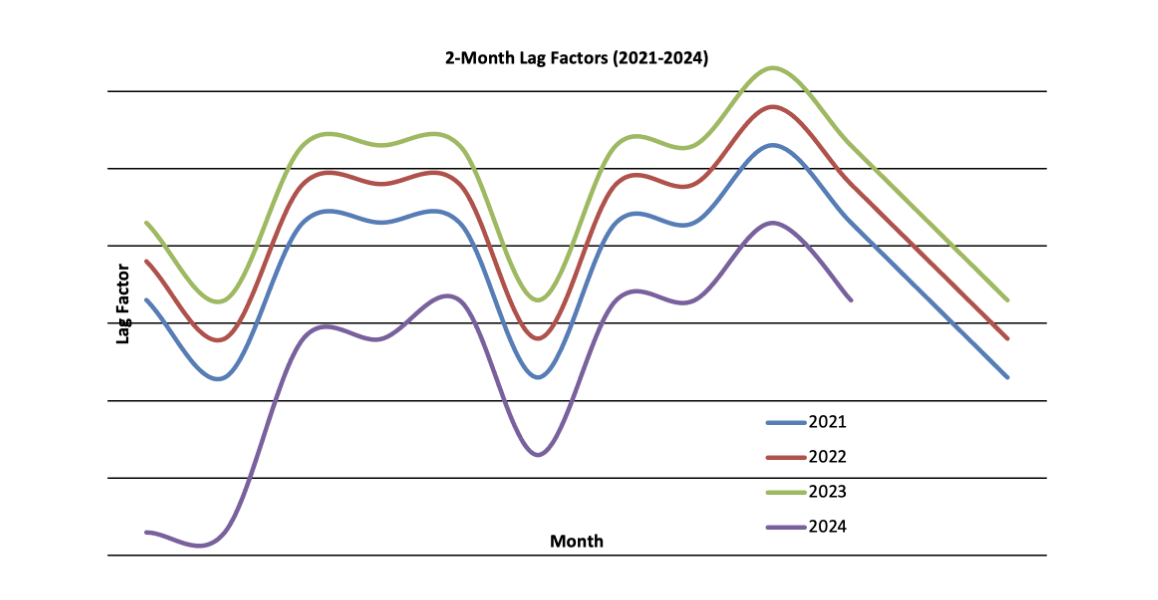
This article is provided for informational and educational purposes only. Neither the Society of Actuaries nor the respective authors’ employers make any endorsement, representation or guarantee with regard to any content, and disclaim any liability in connection with the use or misuse of any information provided herein. This article should not be construed as professional or financial advice. Statements of fact and opinions expressed herein are those of the individual authors and are not necessarily those of the Society of Actuaries or the respective authors’ employers.
Dave Nelson, FSA, MAAA, is an advisor at Havarti Risk. Dave can be reached at dave.nelson.111@gmail.com.
Patrick Getzen, FSA, MAAA, is a strategic advisor at Aphora Health. Patrick can be reached at pgetzen1@gmail.com.
Ron Hulet, ASA, MAAA, is chief strategy officer at Havarti Risk. Ron can be reached at rhulet@havarti-risk.com.

